STIs are rising fast in England. They're rising even faster in Liverpool

On the spike in syphilis and gonorrhoea across Merseyside
Dear members — welcome to The Post, ever the home of glitz and glamour. Today, we’re talking about venereal disease. Statistics show that both syphilis and gonorrhoea are on a dramatic incline in this region — but why? Jack explores in today’s read. We’re aware this is going out early enough that there’s a danger it will coincide with your breakfast. But don’t worry — there’s no unsightly images or gory details below.
But before we get there: Liverpool’s criminal contingent heads to the Isle of Man for better prices, while campaigners attempt to stop an “already heavily polluted borough” from getting worse in our news briefing below.
Your Post briefing
Detectives are cracking down on Liverpool-based criminals exploiting higher drug prices on the Isle of Man. Detective Inspector Jamie Tomlinson, of the Drug and Organised Crime Unit, told the Echo that they were working alongside Merseyside Police to target organised crime groups operating on the famously quiet island. Last week, Kyle Johnson, a Merseyside criminal who operated an elaborate scheme from his prison cell, received a 20 year sentence for plotting to ship Class A and B drugs to the Isle of Man via the postal service. Tomlinson warned of possible misconceptions: “People assume the island is a sleepy hollow, but they don't realise drug prices are a lot higher than the UK so it is big business for drug criminals in the north west.”
Campaigners fighting against plans to build a massive dual carriageway across a country park under the ‘Save Rimrose Valley’ banner marched six miles into Liverpool to highlight their cause. National Highways want to build a £250m access road to the Port of Liverpool, but have become embroiled in an ongoing war with environmental campaigners, who believe the 3.5km park and valley will be destroyed in the process and the “already heavily polluted borough” will see its air quality worsen. The project has currently been pushed back to 2025 at the earliest. If you want to read more in-depth about the Rimrose Valley situation, as well as the broader implications of north Liverpool and south Sefton’s poor air quality, have a read of this fantastic piece by Joel Hansen from April.
A mum in social housing in Liverpool who found large mould patches throughout her house has expressed concern for the safety of her children. 31-year-old Megan Tennant, who lives with her partner, four-year-old son Archie and 14-month-old daughter Orla, told ITV that despite repeated complaints to Onward Homes, the issue is not being fixed. "The work has never been done properly — it has been bodged at every opportunity. The moisture board in my bathroom has rotted away and is full of mould. My son and I have asthma,” she said, adding that the case of two-year old Awaab Ishak, who died of a respiratory condition caused mould in his socially-provided Rochdale flat in 2020, is always on her mind. Onward Homes says it had not found any mould but apologised for any distress.
Post Picks
🎭 Over in Salford, a play about one of the strangest pieces of real-life Liverpool folk mythology, Being Purple Aki, promising “romantic paranoia, surrealism, possession, human frailty and the desperately real need for personal reinvention”. Tickets cost £10.
🏛️ Any tile enthusiasts in the house? Well, a rare opportunity is on offer this month, for tile lovers and tile novices alike — a chance to see the Milton tiles, a grand Victorian mosaic hidden since the 19th century under the wooden floor at St George’s Hall. Have a look.
🛍️ Journey on down to St Luke's Bombed Out Church on Sunday for a vinyl record fair, hosted by some of the city’s best traders. DJs will be spinning tracks from 10am, with live music from the steps at 12pm. The event is free to enter.
In 1673’s ‘A Satire Against Marriage’, the infamously promiscuous Earl of Rochester — John Wilmot, dismissed any concerns about his frequenting large numbers of prostitutes, stating: “the worst you can fear is but a disease,/And diseases, you know, will admit of a cure.” Wilmot died at the age of 33 after complications arising from syphilis.
Much has changed since the 1600s. Rakish libertines no longer roam the streets of the capital, and thankfully syphilis is no longer a major killer. Nonetheless, the infection, generally associated with early modern or even medieval England, has made something of a comeback. Cases across the country have been on a sharp incline, reaching the highest levels seen since the years following the Second World War, and locally we’ve seen them more than quadruple in a decade.
And it isn’t only syphilis. Gonorrhoea has seen an even more notable increase locally — up 113% between 2021 and 2022. That puts Liverpool 17th in England, with a ratio of 311.9 cases per 100,000 people. Wirral saw an even bigger rise, 135%, and for Sefton and St Helens it was 73% and 72% respectively. The caveat hanging over all of this is that as testing increases, and sexual health organisations improve at targeting their testing to the most relevant parts of the population, more cases will inevitably be picked up. But even when you take that into consideration, the current numbers are raising eyebrows in clinics across the region.
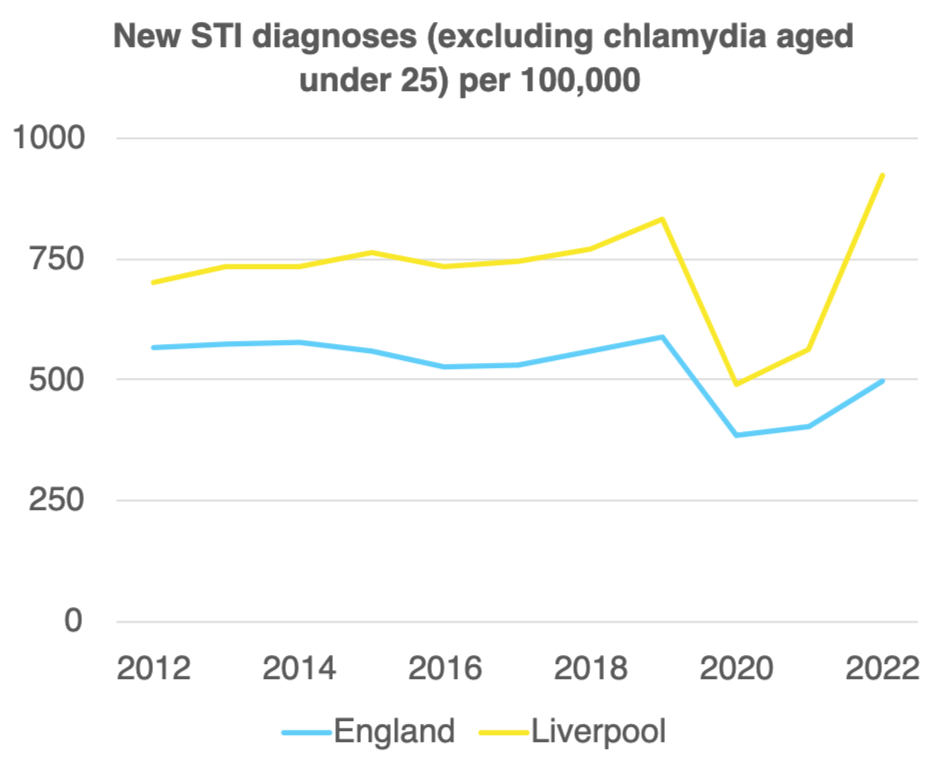
The interesting question is whether there are specific local factors driving this. Because yes, England is seeing a dramatic STI spike, but ours is — well — a touch more dramatic. While the national rate per 100,000 people for new STIs was at 495.8 per 100,000, Liverpool is considerably higher at 922.0 cases per 100,000 of the population. Our current rates are not far off twice the national average then. So why might it be that our line on the graph is trending up so dramatically?
Ant Hopkinson is the CEO of Sahir House, a charity providing frontline LGBTQ+ support services, including sexual health services. To Hopkinson, a number of factors are at play here, local and national, but the overriding one is obvious: the accessibility of PrEP. PrEP, or pre-exposure prophylaxis, is a preventative drug taken to protect yourself against the threat of HIV. Given the primary communities seeing an increased number of cases are gay and bisexual men (who account for 69% of total cases), it’s the theory that makes the most sense.
Dr Anatole Menon-Johansson — who works at Brook, a nationwide sexual health charity with a Wirral base — explains the root of the problem: “People used to wear condoms to protect themselves against HIV but nobody’s worried about HIV anymore. And for good reason”. PrEP isn’t 100% effective (trials have put it closer to 86%, Dr Menon-Johansson tells me) but it certainly has the general effect of making people feel safe against the major threat. “When you give someone PrEP and try to give them condoms, they sometimes don’t want the condoms,” Menon-Johansson says.
This is a strange paradox to be caught in. You create an effective defence against one extremely serious infection, but by doing so you lower your defences against a number of less serious ones. As Menon-Johansson says, “you win some, you lose some”.
And, as everyone I speak to is keen to stress, “less serious” doesn’t mean “not serious at all”. Syphilis — left untreated — can lead to stillbirth for pregnant women, nerve or memory problems and even damage to organs. It is uncommon for things to get this bad, but it can happen.
Part of the difficulty here is getting the message across in a way that doesn't demonise the LGBTQ+ community. “I really don’t want to ghettoise the entire LGBT community,” Hopkinson says. The whole community can get attacked whenever we see a spike.” Suffice to say, there’s history here when it comes to public health panics regarding infection. “When monkeypox became a thing in the media, the rhetoric was around how the LGBT community was disproportionately affected,” Hopkinson says. “Some of the reporting echoed back to the 80s and HIV”. These kinds of panics, he says, tend to only gain traction with emerging health crises. A spike in an infection is less likely to raise alarm bells, or pique the interest of tabloid journalists.

Not everyone is fully sold on the PreP narrative though. A doctor from Axess, a free sexual health service in the north west, tells me that “in general people on PreP are quite engaged with their sexual health.” She adds that their internal data doesn’t point to PreP being the cause. According to her, it’s more simple. The young population in Liverpool (roughly five years below the national average, in part due to the large number of students) is a factor, given STIs are most common in 16-24 year olds, plus socio-economic factors, Liverpool — more broadly Merseyside — has a number of highly deprived areas.
The increased testing can’t be understated either, she says. During COVID home testing became more common, and the services across the borough have generally been reconfigured to make them more streamlined. Liverpool has a number of places people can access testing easily, whereas some parts of the country are currently looking at lengthy wait times. In such circumstances, some people end up not bothering. Again, it’s something that could skew the results. “The really important thing is that people locally are taking their sexual health seriously and testing more,” she says.
Dr Bobby Ahmed, CEO and Medical Director at the private Regent Street Clinic (which has a clinic in Liverpool) doesn’t think the PrEP narrative tells the whole story either though. At least, not in younger subsets of the population, anyway. He tells me his clinic used to see three or four cases of gonorrhoea annually, now he’s seeing two or three a week, with particularly alarming rates among young people. “I don’t think that’s all to do with PrEP and HIV. Young people never ever mention it — it's definitely there for an older generation, but for young people that message is dated now”.
Ahmed thinks focusing on behavioural changes instead is key. Coming out of the pandemic he saw “a change in people’s mentality; more freedom, celebratory, perhaps more risk-taking behaviour”. This created a roaring 20s effect of sorts — an unshackling. And Ant has always seen behavioural changes too, a “rise in public sex, cruising and dogging alike have increased” he says, although none of this has a particular regional slant.

The pandemic has also played its part in another way. “Coming out of COVID I met women who were going into sex work because their regular jobs were unavailable,” Menon-Johansson says. This is purely anecdotal, but it stands to reason that financial pressures due to decreased wages would have pushed women towards sex work. The Financial Times reported on this late last year. They found a steep rise in escort services as cost of living pressures rose, and that customers “emboldened by their newfound market power — are becoming more demanding”. As the HIV campaigning group Sophia Forum point out, sex workers are often under pressure to have sex without a condom (and so they advocate for male and female sex workers alike to take PrEP).
Of course this isn’t only a behavioural thing though. There has also been what Ahmed describes as a “relative decommissioning” of sexual health services in the UK in the past decade. “Ten years ago if you’d had unprotected sex and you were worried you could get into your local GMU clinic. You’d just make a phone call or even walk in,” he adds. “Now, if you try to access a GMU clinic you often clinically can’t get an appointment”.
Sexual health spending is ring-fenced by local government. And as local governments all across the country have made cuts in the past 10 years, sexual health has often been an easy target. Take Wirral as an example. Between 2013 and 2022 Wirral’s services saw cuts of £400,000. All the while, the number of people catching STIs increased. Between 2021 and 2022 alone gonorrhoea cases more than doubled and syphilis spiked. There is some good news, at least in Wirral’s case. After a recent report warned sexual health services in Wirral were almost at “breaking point”, a new contract has been approved by the council, marking a large increase in sexual health spending with a £21.1 million contract for up to seven years. It’s needed.
Menon-Johansson says he’s often made the argument that the “return on investment” with regards to sexual health services is high. For every £1 spent on contraception it’s said the NHS saves £13. For every £1 on HIV testing the NHS saves £2.50. “You have to spend money to save money. A lot of work upstream is prevention work, to reduce downstream spend. This is true of so many things”. It’s a point echoed by everyone I speak to.

The Earl of Rochester’s unfortunate fate is unlikely to befall the 21st century sufferers of syphilis, and we can be thankful for that. But at the end of his poem ‘The Disabled Debauchee’ (the tale of a “brave admiral” and his “honourable scars” — I’ll let you guess what he’s alluding to there) he does offer us a warning: “And being good for nothing else, be wise”. Perhaps what he meant was to not make the same mistakes as him, and to pop down to the clinic.

Comments
Latest
Exclusive: New documents claim Big Help’s bosses owe over £17mn
Liverpool is still trapped in a crime drama Cage
Farage is targeting Sefton council. Locals aren’t so sure
'Demoralised and lied to': Inside the NHS cuts nobody sees
STIs are rising fast in England. They're rising even faster in Liverpool
On the spike in syphilis and gonorrhoea across Merseyside